Blood is connective tissue, flowing through capillaries, veins, and arteries in all vertebrates. The red color is characteristic due to the presence of hemoglobin in the red blood cells.
Blood is an essential fluid that sustains life by performing various biochemical functions. It serves as the primary medium for transporting oxygen, nutrients, hormones, and immune cells throughout the body, ensuring homeostasis and optimal physiological activity. Additionally, blood plays a key role in the elimination of metabolic waste, regulation of pH, and defense against infections.
Understanding the biochemical composition of blood is crucial for diagnosing diseases, monitoring health status, and advancing medical research. Clinical biochemistry reveals the molecular mechanisms of various physiological and pathological conditions by analyzing the components of blood in detail.
Why Study Blood Biochemistry?
Biochemical blood analysis helps in:
- Identifying metabolic disorders
- Assessing organ function, including the liver and kidneys
- Diagnosing and monitoring diseases such as diabetes, cardiovascular conditions, and cancer
- Evaluating the immune system’s response to infections
- Understanding the impact of lifestyle choices on health
By examining blood composition and its biochemical properties, healthcare professionals can develop precise treatment strategies and improve patient outcomes.
Basic Composition of Blood
Cells and an extracellular matrix combine to form blood, a dynamic tissue essential for physiological functions. These two primary fractions—the cellular component and the blood plasma fraction—work together to maintain homeostasis, transport nutrients, and facilitate immune defense.

a. Cellular Fraction: The Formed Elements
The formed elements, also known as figurative elements, include semi-solid and particulate components suspended in plasma. These elements consist of
- Red Blood Cells (Erythrocytes): Oxygen carriers responsible for gas exchange.
- White Blood Cells (Leukocytes): Immune cells that protect against infections.
- Platelets (Thrombocytes): Essential for blood clotting and wound healing.
These cell-derived components originate in the bone marrow, ensuring continuous renewal to maintain circulatory efficiency.
b. Plasma Fraction: The Extracellular Matrix
Blood plasma is a translucent, yellowish liquid that serves as the extracellular matrix where cellular components remain suspended. It plays a crucial role in:
- The process involves the transport of nutrients and waste between cells and organs.
- Maintaining electrolyte balance ensures that biochemical reactions occur efficiently.
- The distribution of hormones regulates metabolism and bodily functions.
Plasma maintains an isotonic environment for blood cells, preventing osmotic imbalances. It is similar in concentration to physiological saline (0.9% NaCl), ensuring cell survival and stability.
c. Blood Composition Ratio: Cellular vs. Plasma Fraction
- Formed elements account for approximately 45% of total blood volume. Red blood cell mass primarily influences the measurement of this proportion, known as the hematocrit.
- Blood plasma comprises 55% of blood volume, acting as the acellular fraction, essential for transporting dissolved substances.
Together, these components create a functional circulatory system that supports oxygen transport, immune defense, clot formation, and homeostasis.
1. Plasma: The Liquid Medium / The Extracellular Matrix
Blood plasma is a translucent, yellowish liquid that serves as the extracellular matrix where cellular components remain suspended. It plays a crucial role in:
- The process involves the transport of nutrients and waste between cells and organs.
- Maintaining electrolyte balance ensures that biochemical reactions occur efficiently.
- The distribution of hormones regulates metabolism and bodily functions.
Plasma maintains an isotonic environment for blood cells, preventing osmotic imbalances. It is similar in concentration to physiological saline (0.9% NaCl), ensuring cell survival and stability.
Plasma constitutes approximately 55% of the total blood volume, acting as a carrier for cells, nutrients, hormones, and waste products. It is composed of
- Water (90%): The primary solvent that facilitates biochemical reactions and transports substances.
- Proteins (8%): They are essential for supporting immunity, facilitating blood clotting, and maintaining osmotic balance. The key plasma proteins include
- Albumin: It regulates blood pressure and transports molecules.
- Globulins: They help in immune defense and enzymatic functions.
- Fibrinogen: Essential for blood clot formation.
- Electrolytes (sodium, potassium, calcium, chloride, and bicarbonate) help to maintain pH balance, nerve function, and fluid regulation.
- Hormones and Enzymes: Regulate metabolism, organ function, and cellular communication.
- Nutrients (glucose, lipids, amino acids, and vitamins) provide energy and support to the tissue growth.
- The kidneys and lungs transport metabolic waste, which includes urea, carbon dioxide, and lactic acid.
2. Cellular Components of Blood/Blood Cells (Hematocytes)
The cellular portion of blood comprises around 45% of total blood volume and consists of the following major components:
Red Blood Cells (RBCs) / Erythrocytes
Red blood cells, commonly known as RBCs or erythrocytes, are a vital part of the circulatory system. They are responsible for carrying oxygen from the lungs to the body tissues and returning carbon dioxide from the tissues back to the lungs. RBCs make up nearly 40–45% of the total blood volume.
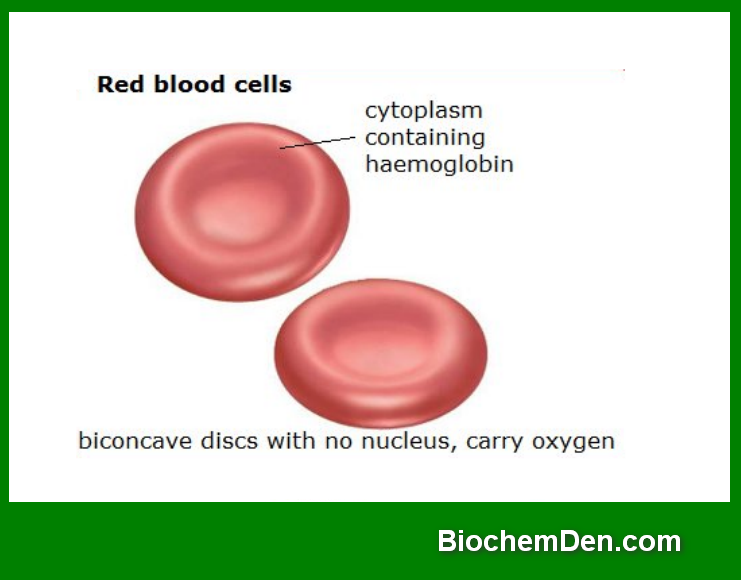
Key Characteristics of Red Blood Cells
| Feature | Description |
|---|---|
| Shape | Biconcave disc (doughnut-like without a hole) |
| Size | About 6-8 micrometers in diameter |
| Nucleus | No nucleus (anucleate) |
| Cytoplasm | Contains a red pigment called hemoglobin |
| Lifespan | Around 120 days |
| Production site | Red bone marrow (in adults) |
| Destruction site | Mainly in the spleen (also known as the graveyard of RBCs) |
| Count (average) | Around 4.5 to 5.5 million per microliter of blood |
Structure and Features
- Shape: Biconcave disc (doughnut-like with a central depression)
- Size: Approximately 6–8 micrometers in diameter
- Nucleus: It is absent and allows more space for hemoglobin
- Color: Red, due to the presence of hemoglobin
- Flexibility: Can squeeze through tiny blood vessels (capillaries)
Composition
- Hemoglobin: The iron-rich protein that binds with oxygen and gives blood its red color. One hemoglobin molecule can carry four oxygen molecules.
- No Organelles: Red blood cells (RBCs) lack a nucleus, mitochondria, and other organelles, which maximizes space for hemoglobin and enhances their oxygen-carrying capacity.
Functions of RBCs
- Oxygen Transport: Hemoglobin binds with oxygen in the lungs and delivers it to tissues throughout the body tissues. Each hemoglobin molecule can carry 4 oxygen molecules.
- Carbon Dioxide Transport: It helps carry carbon dioxide from the body’s tissues to the lungs for exhalation. About 20–25% of carbon dioxide is carried by hemoglobin.
- Maintains pH: Assists in buffering the blood’s pH level through hemoglobin and carbonic anhydrase.
Hemoglobin (Hb)
- Hemoglobin is the iron-containing protein in RBCs that binds with oxygen.
- Normal values:
- Men: 13.5–17.5 g/dL
- Women: 12.0–15.5 g/dL
- Hemoglobin also gives red blood cells their distinct red color.
RBC Formation: (Erythropoiesis)
- RBCs are produced in the red bone marrow through a process called erythropoiesis.
- This process is regulated by the hormone erythropoietin, which is released by the kidneys in response to low oxygen levels.
- The entire maturation process takes around 7 days.
Lifespan and Destruction
- Average lifespan: About 120 days
- The spleen, also known as the “graveyard of RBCs,” removes old RBCs.
Normal Count in Blood
- Men: 4.7 to 6.1 million cells/µL
- Women: 4.2 to 5.4 million cells/µL
- Children: 4.1 to 5.5 million cells/µL
Disorders Related to RBCs
| Condition | Description |
|---|---|
| Anemia | A low RBC count or hemoglobin can cause fatigue and weakness. |
| Polycythemia | An abnormally high RBC count raises the risk of clotting. |
| Sickle Cell Anemia | Hemoglobin production is affected by a genetic condition. |
| Thalassemia | Genetic condition affecting hemoglobin production. |
Summary
- RBCs are oxygen carriers with a biconcave shape and no nucleus.
- It contains hemoglobin, the key protein for gas exchange.
- Main function: Transport of oxygen and carbon dioxide.
- Lifespan: 120 days; produced in red bone marrow.
- Disorders include anemia, sickle cell disease, and polycythemia.
Red Blood Cells are the workhorses of the circulatory system. Their unique structure and hemoglobin content make them perfect oxygen carriers. Understanding RBCs is essential for grasping how our body functions and for acing your exams in biology and human physiology.
White Blood Cells (WBCs) / Leukocytes
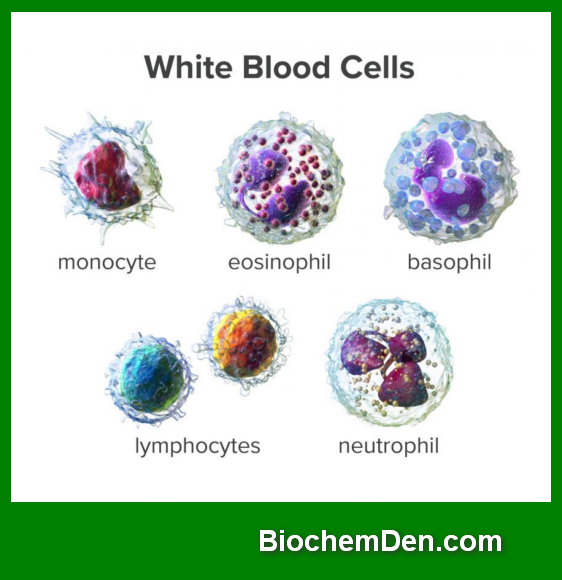
White blood cells (WBCs), also known as leukocytes, are an essential part of the body’s immune system. Unlike red blood cells, WBCs do not contain hemoglobin and are fewer in number, but they play a powerful role in defending the body against infections, foreign invaders, and abnormal cells.
Key Characteristics of WBCs
| Feature | Description |
|---|---|
| Shape | Irregular (amoeboid) movement through tissues |
| Size | Larger than RBCs (12–17 micrometers) |
| Nucleus | Present (single or multi-lobed) |
| Color | Colorless (appear white in centrifuged blood sample) |
| Mobility | Capable of movement (can squeeze through capillary walls) |
| Count | 4,000 to 11,000 cells per microliter of blood (normal range) |
Types of White Blood Cells (WBCs) / Leukocytes
Based on the presence or absence of granules in their cytoplasm, white blood cells fall into two main categories:
1. Granulocytes (With Granules)
Granulocytes are WBCs that contain visible granules in their cytoplasm and have lobed nuclei. As part of the innate immune system, they serve as the initial line of defense.
a) Neutrophils
- Most abundant WBCs (60–70% of total WBC count)
- Nucleus: Multi-lobed (usually 3–5 lobes)
- Cytoplasm: Contains fine, pale granules
- Function:
- First responders to bacterial and fungal infections
- Engulf pathogens through phagocytosis
- Form pus at infection sites
- Lifespan: 6 hours to a few days
b) Eosinophils
- Make up about 2–4% of WBCs
- Nucleus: Bi-lobed
- Cytoplasm: Contains large, red-orange granules
- Function:
- Fight parasitic infections (especially worms)
- Involved in allergic reactions (like asthma)
- Regulate inflammation
- Fun Fact: Eosinophil count rises during parasitic infestations.
c) Basophils
- Least common WBCs (<1%)
- Nucleus: S-shaped or lobed (often obscured by granules)
- Cytoplasm: Contains large, dark purple granules
- Function:
- Release histamine and heparin during allergic and inflammatory responses
- Histamine causes vasodilation (widening of blood vessels)
- Heparin prevents blood clotting at the site of inflammation
2. Agranulocytes (Without Granules)
Agranulocytes have no visible granules in their cytoplasm and a non-lobed, large nucleus. They are crucial for adaptive immunity.
a) Lymphocytes
- Make up 20–25% of WBCs
- Nucleus: Large, round, and occupies most of the cell
- Types:
- B lymphocytes (B cells): Produce antibodies to neutralize antigens
- T lymphocytes (T cells): Destroy infected or cancerous cells; regulate immune response
- Natural Killer (NK) cells: Attack virus-infected and tumor cells
- Function:
- Provide long-term immunity
- Recognize specific pathogens (part of adaptive immunity)
- Lifespan: Weeks to years (some memory cells last a lifetime)
b) Monocytes
- Make up 3–8% of WBCs
- Nucleus: Large, kidney- or horseshoe-shaped
- Largest type of WBC
- Function:
- Migrate into tissues and become macrophages
- Perform phagocytosis to clean up debris, dead cells, and microbes
- Present antigens to lymphocytes to trigger adaptive immune responses
- Lifespan: Days in the blood, months as macrophages in tissues
Quick Summary Table
| Type | Subtype | Main Function | % in Blood |
|---|---|---|---|
| Granulocytes | Neutrophils | Phagocytosis: become macrophages | 60–70% |
| Eosinophils | Kill parasites, modulate allergic reactions | 2–4% | |
| Basophils | Release histamine, initiate allergic response | <1% | |
| Agranulocytes | Lymphocytes | Antibody production (B cells), immunity (T cells) | 20–25% |
| Monocytes | Phagocytosis; become macrophages | 3–8% |
Exam Tip
- Neutrophils = Numerous
- Eosinophils = Allergies + Parasites
- Basophils = Baseline of allergy (histamine)
- Lymphocytes = Long-term immunity
- Monocytes = Massive macrophages
c. Platelets / Thrombocytes
Platelets, also known as thrombocytes, are small, disc-shaped cell fragments found in the blood. Unlike red and white blood cells, platelets do not have a nucleus, but they play a critical role in blood clotting and wound healing.
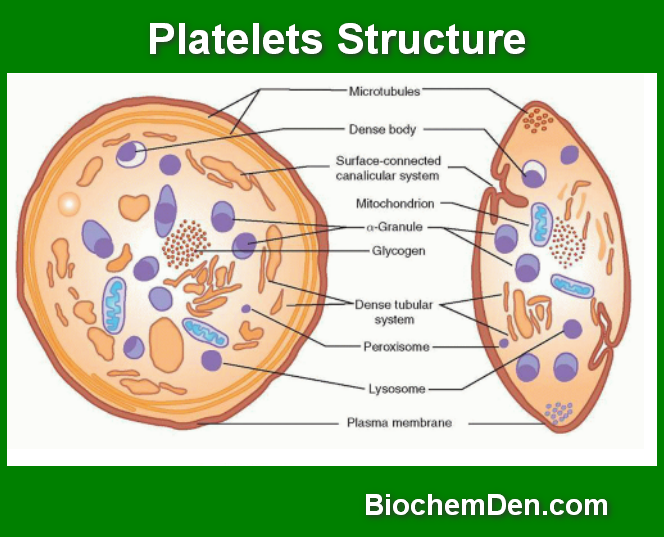
Key Characteristics of Platelets
| Feature | Description |
|---|---|
| Shape | Small, irregular, disc-shaped |
| Size | 2–4 micrometers in diameter |
| Nucleus | Absent |
| Origin | Produced from megakaryocytes in the red bone marrow |
| Count | 150,000–450,000 per microliter of blood (normal range) |
| Lifespan | 7 to 10 days |
Formation of Platelets: (Thrombopoiesis)
- Platelets are formed in the red bone marrow from megakaryocytes, which are large cells.
- These megakaryocytes break into thousands of tiny fragments, which become platelets.
- This process is regulated by a hormone called thrombopoietin.
Functions of Platelets
- Blood Clotting (Coagulation):
Platelets gather at the site of a blood vessel injury, stick together (platelet plug), and release clotting factors that help form a blood clot. - Prevention of Blood Loss:
By forming clots, platelets help seal wounds and prevent excessive bleeding. - Wound Healing:
They release growth factors that help repair damaged tissues and promote healing.
Platelet Activation Process
When a blood vessel sustains damage,
- Adhesion: Platelets stick to the exposed collagen of the damaged vessel wall.
- Activation: They change shape and release chemical signals (like ADP and thromboxane A2).
- Aggregation: Platelets stick to each other and form a temporary plug.
- Clot Formation: With the help of fibrin (a protein), a stable blood clot forms.
Abnormal Platelet Count – What It Indicates
| Condition | Meaning |
|---|---|
| Thrombocytopenia | Low platelet count – causes excessive bleeding, bruising |
| Thrombocytosis | High platelet count – may lead to unwanted blood clots |
Quick Revision for Exams
- Platelets are cell fragments with no nucleus and help in clot formation.
- Origin: Megakaryocytes in bone marrow.
- Normal count: 1.5–4.5 lakh/µL (150,000–450,000/µL).
- Lifespan: 7–10 days.
- Key function: Prevent bleeding by forming clots.
Did You Know?
- The spleen removes platelets from the body when they age or sustain damage.
- People with very low platelet counts may suffer from a condition called hemophilia (though true hemophilia is due to clotting factor deficiencies, not platelets directly).
- Platelet transfusions are used for patients with severe bleeding or undergoing chemotherapy.
Platelets may be small, but they’re life-saving components of blood. Understanding their role is crucial for students preparing for biology or medical entrance exams and anyone curious about how our body prevents blood loss after injury.
Conclusion
Blood is a complex and dynamic fluid that plays a fundamental role in sustaining life. Its cellular and extracellular components work together to transport oxygen and nutrients, regulate immune responses, maintain homeostasis, and facilitate waste removal.
The formed elements—red blood cells, white blood cells, and platelets—ensure oxygen distribution, immune defense, and clot formation. Meanwhile, plasma serves as the extracellular matrix, carrying essential substances like proteins, electrolytes, hormones, and metabolic waste, ensuring biochemical stability throughout the body.
Understanding blood composition is crucial in medical diagnostics, disease prevention, and therapeutic advancements. From identifying hematological disorders to developing innovative treatment strategies, blood remains an invaluable focus of scientific research and clinical practice.
As knowledge of blood biochemistry continues to evolve, its applications in personalized medicine, biotechnology, and regenerative therapies will further enhance healthcare and disease management. The study of blood composition deepens our understanding of human physiology and sets the stage for future innovations in medical science.
Discover more from Biochemistry Den
Subscribe to get the latest posts sent to your email.





